A group of orthopaedic surgeons believes that operating and clinic times are not used efficiently in their hospital. They believe their chief is unapproachable and does not dedicate time during departmental meetings to bring forward issues of concern to the staff. They see his decisions as “top down” and not patient-centred. The staff feel powerless to address the issue. They wonder, “How are we supposed to provide safe care as a department, when our chief won’t let us help him?”
From his vantage point, the chief of orthopaedics has concerns about his team’s performance. He describes his team as “negative” and “critical” and deplores that the surgeons “just won’t do as I tell them.” He feels that the physicians in the department “just don’t understand” the hospital politics that drive his decisions and wonders what he could do to “get the team to gel.”
Could fostering psychological safety help the chief of orthopaedics in the vignette be a more influential and impactful leader?
Psychological safety can be defined as a shared belief that anyone on the care team can speak up, sharing their opinion respectfully and without fear of retribution.1 It is indispensable in medicine as the sharing of experiences is necessary to reduce patient safety risks and learn from patient safety incidents or near-misses.
Psychological safety is also an essential element of the Institute of Healthcare Improvement’s (IHI) Framework for Safe, Reliable, and Effective care (see Figure 1).2 The framework conceptualizes highly reliable healthcare delivery systems as a series of interconnected elements that you, as a physician leader, can leverage to deliver safe care. With your influence on an organization’s culture and learning systems, you are uniquely positioned to nurture teams that provide highly reliable care.3
Previous CMPA articles explore components of the IHI framework including leaders’ role in fostering safe and reliable care, as well as the elements of a just culture and natural justice.3,4,5 This article explores psychological safety.
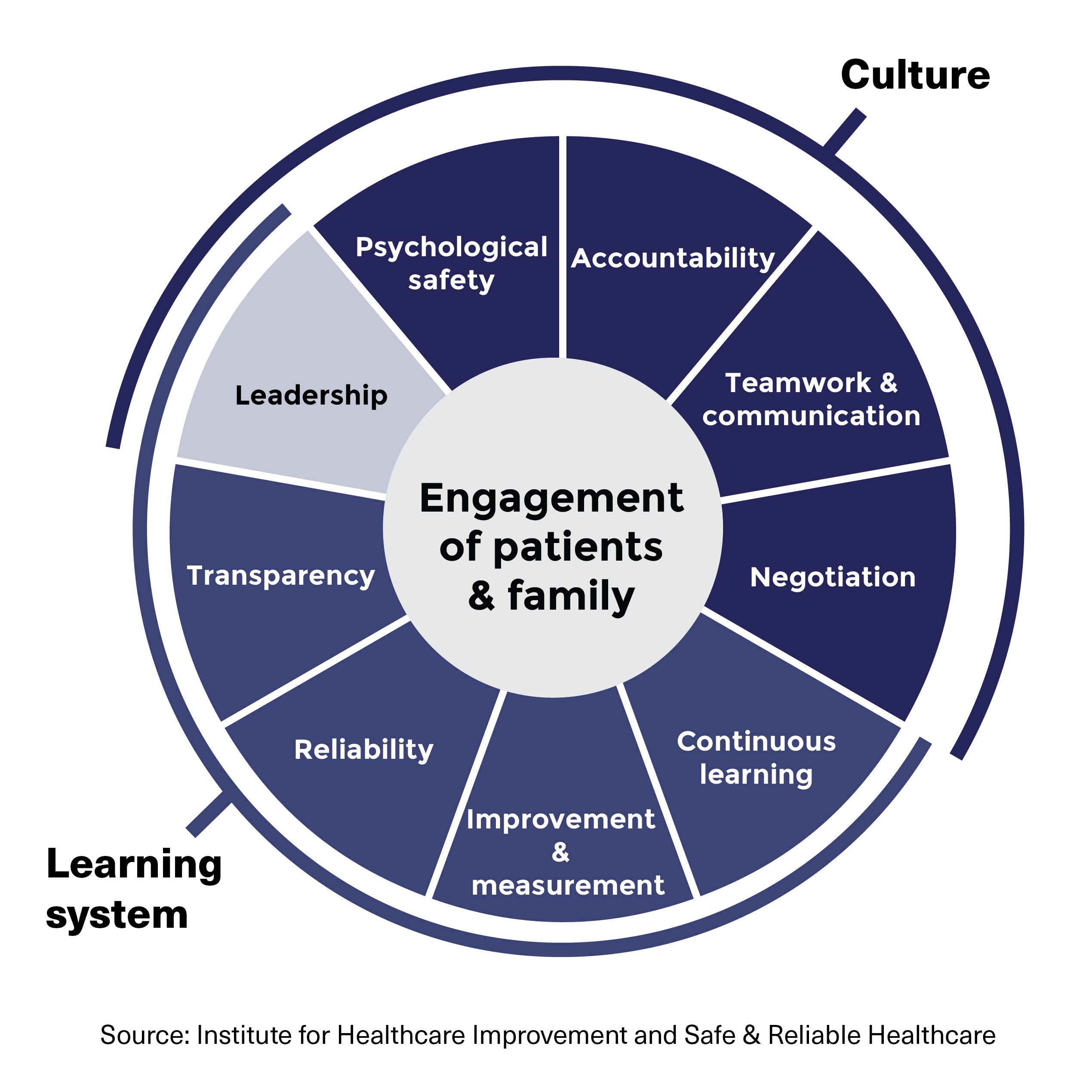 Figure 1: Framework for Safe, Reliable, and Effective Care
Figure 1: Framework for Safe, Reliable, and Effective Care
Describing psychologically safe environments
In psychologically safe environments, all members of a healthcare team feel safe when they propose improvements and innovations. As well, learning is accomplished as much “in the moment” as it is “after the fact” because team members can:
- ask questions without fear of being labelled ignorant
- ask for feedback without fear of being considered incompetent
- make a suggestion without fear of being branded negative
- be respectfully critical without fear of being regarded as disruptive
Situational awareness defined
6
Situational awareness is the acquisition and understanding of the dynamic information present in the environment. It involves keeping track of what is happening and anticipating what might need to be done or adapted as a result.
In psychologically safe environments, people contribute to the creation of a shared team situational awareness. All team members are confident their colleagues would never embarrass or punish anyone else for making a mistake and they are reassured that any event will be seen as an opportunity to learn. Team members are encouraged to ask questions, admit a vulnerability, or offer suggestions. They are confident their suggestions will truly be considered and, if appropriate, acted on. When suggestions are not acted on, team members know leaders will explain the reasons for the decisions.
Benefits of psychological safety
7
- encourages speaking up
- enables clarity of thought
- supports productive conflict
- mitigates failure
- promotes innovation
- increases accountability
Psychological safety starts with leaders
Psychological safety allows the melding of continuous learning with high performance. As an organizational mindset, it focuses on ensuring that an organization’s learning processes promote safe care and continue to evolve to do so as best as possible. It is difficult for organizations to proactively address identified vulnerabilities when frontline healthcare providers do not feel psychologically safe to speak up to their leaders, let alone to one another.
Psychological safety does not occur by decree. While directives, guidelines, and slogans can communicate a leader’s intent to foster psychological safety, they do not create it. For psychological safety to take hold and grow, you must explicitly promote it, model it, and continually mentor others to espouse it.
Three steps to psychological safety
As a leader, you can take three practical steps to help establish psychological safety within a team:
- Promote healthy conflict
- Encourage speaking up
- Use the platinum rule
1. Promote healthy conflict
Many people find it uncomfortable to disagree with others and suggest a different way forward. The problem with conflict is not that it occurs, but rather the meaning people attribute to it in the moments that follow. It is the interpersonal fear that their leader or a colleague will be angry about the comment or question—born of a lack of psychological safety—that can dominate the workplace and hinder the collaboration that is required to provide safer care.
You can help normalize respectful conflict and foster a sense that all team members are valued by including clear expectations for and support of respectful workplace discussions. By reassuring the group that your ultimate goals are patient safety and quality improvement, and by making clear that you will not tolerate behaviours that belittle, embarrass, or ostracize team members, you can set the stage for healthy discussions.
2. Encourage speaking up
Patient safety incidents are frequently due to a complex set of contributing factors (e.g. cognitive overload or unconscious drift away from safe practices). This complexity can often make it difficult for individuals to recognize they are about to commit an error leading to a patient safety incident until the error has occurred. While individuals may be blind to their errors, their co-workers may see and hear things differently, and may recognize an otherwise unappreciated risk. When co-workers speak up about their concerns, it is a form of respectful, yet candid communication.
Fear of offending someone perceived as higher up in the hierarchy is widespread in healthcare. Because of this fear, coworkers often hesitate to say something, even when they think a situation may present a risk. As a physician leader, you can foster speaking up by inviting it frequently and openly. Using statements like “I may miss things so if you see me do something that might impact patient safety, please tell me” opens the door. Repeated invitations are as important as the words used to create psychological safety.5
Being candid about your limitations and honestly inviting others to speak up sends a powerful signal about establishing a speaking up culture. However, it’s perhaps even more important to model listening up. Acknowledging someone’s courage to speak up and acting on the shared information appropriately shows that you are “walking the talk” and it enhances your credibility.
To best predict whether individuals will speak up, look at the response they received the last time they spoke up. If you want to encourage speaking up, congratulate those who do—especially when the concern raised is ultimately felt to be ill-founded. Doing this models the appropriate response and demonstrates your willingness to be vulnerable.
3. Use the platinum rule
The golden rule states, “Treat others as you would want to be treated.” When it comes to psychological safety, however, the platinum rule prevails: “Treat others as they would want to be treated.”
Healthcare providers want to contribute and make a difference. By encouraging frontline providers—those doing the work and intimately familiar with the issues—to share their ideas and propose solutions, you can operationalize and enhance your departmental vision, whatever it may be.
Leaders who are unable or unwilling to receive feedback from others and turn it into meaningful action often silence those below them in the hierarchy. However, using good listening skills, you can inoculate healthcare workers against self-censorship and prevent a reflexive tendency to endorse in favour of honest questioning.
You can create psychologically safe environments by reserving your thoughts, asking others about their opinions and preferences, and taking part in discussions about the type of feedback people would like to receive. This approach explicitly communicates your respect for people and an openness to creating an environment where people are valued and bring their best effort to the work they do.
The bottom line
In a high-stakes environment like healthcare, tensions can be expected. As the physician leader, you can transform workplace tensions into teachable moments by fostering and supporting psychological safety. Leveraging such teachable moments promises to increase accountability, enhance system safety, and organize the workplace to truly support learning.
References
- Edmondson, AC. Psychological Safety and Learning Behavior in Work Teams. Admin Sci Q. 1999 Jun;44(2):350-83 doi:10.2307/2666999
- Frankel A, Haraden C, Federico F, et al. A Framework for Safe, Reliable and Effective Care. White paper. Institute for Healthcare Improvement and Safe & Reliable Healthcare;2017
- Canadian Medical Protective Association. CMPA;2018 Jun. Leadership Essentials, How Physician Leaders can nurture Teams that Provide Highly Reliable Healthcare [cited 2020 Apr 2]
- Canadian Medical Protective Association. CMPA;2018 Sep. Leadership Essentials, Creating a Culture of Accountability [cited 2020 Apr 2]
- Boivin D, Lefebvre G, Bellemare S. Natural Justice and Alternative Dispute Resolution: Their Importance in Managing Physician Performance. Can J Physician Leadersh. 2019;6(2):46-50
- Good Practices Guide. Canadian Medical Protective Association. Situational Awareness, What is going on around you? [cited on 2020 Apr 2]
- Edmondson, AC. Teaming: How Organizations Learn, Innovate, and Compete in the Knowledge Economy. Kindle Edition. Jossey-Bass;2012 Mar 16 [cited on 2020 Apr 2]